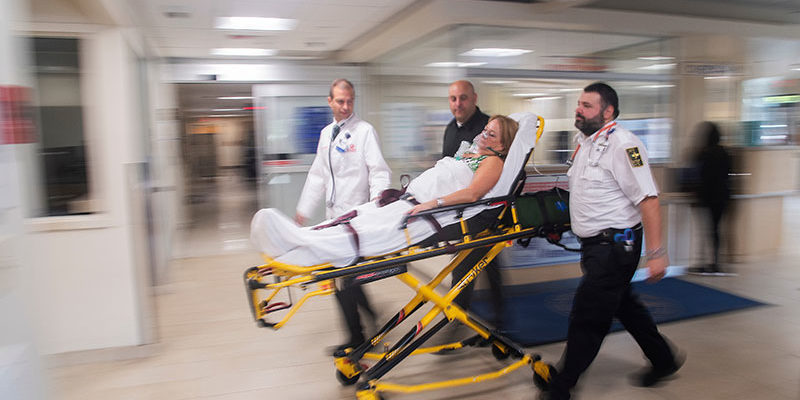
 Emergency Departments (ED) are busy places, filled with people who have a range of medical problems. Not understanding how ED’s work can be confusing and somewhat frustrating. So we put together a list of our frequently asked questions and had our ED professionals respond.
Emergency Departments (ED) are busy places, filled with people who have a range of medical problems. Not understanding how ED’s work can be confusing and somewhat frustrating. So we put together a list of our frequently asked questions and had our ED professionals respond.
Q: What happens when I get to the Emergency Department?
A: You will meet with the nurse in triage. That’s the first step. Depending on your condition you will then be brought to a treatment area right away or, after triage, directed to start the registration process. At pique volume hours, Mather also has a physician or physician assistant in triage to help with the increased number of patients.
-Julie Tegay, BSN, RN-BC, Nurse Manager, Emergency Department
Q: Why is another patient who came in after me being treated first?
A: Every patient is evaluated based on the Emergency Severity Index, a national classification system that determines the acuity of patients’ health care problems and the number of resources their care is anticipated to require. By resources I am referring the types of interventions or diagnostic tools, above and beyond physical examination, such as imaging studies, blood tests, sutures, and intravenous or intramuscular medications. The more life-threatening or emergent your symptoms, the higher you rank on the Index, so interventions are implemented immediately to save your life. Our goal is to treat all patients in a timely manner based on the severity of their illness or injury.
-Phillip Messina, RN, Assistant Vice President of Nursing
Q: How long will I have to wait to be seen?
A: We’ve worked very hard and made changes to keep the time you spend in the ED to a minimum. Since January our door to ED bed placement time has been cut in half. The time it takes for a patient to see a provider after he or she has been placed in an ED bed is seven minutes, well below the national average of 15 minutes.
Earlier this year we placed a physician or physician’s assistant in triage during our busiest times. By doing this, we get immediate insight to what the problem is and initiate workup based on that encounter. That’s been very successful in reducing the time patients spend in the Emergency Department.
The ED also added a second nurse to the triage area. This allows us to provide medication sooner or contrast that may be needed for a CT exam.
-Adam Wos, MD, Medical Director, Emergency Department
Q: Why do ED visits take a long time?
A: Coming to an Emergency Department is very different than having an appointment at your doctor’s office. We are staffed and equipped to handle patients with life threatening conditions to patients with lacerations and sprains. We never know how many people will be coming in at any time or the severity of their medical problems. Mather is constantly looking at processes to improve the patient experience including the time it takes to diagnose and admit or treat and release our patients.
As an ED patient, your physician will want to order tests on you. Obtaining all the test results may take some time. We’re doing everything we can to expedite your care. If you have any questions about your wait time just ask anyone and they’ll provide you with an estimate.
Once we have all the test results back, the physician can determine the course of treatment and whether you will need to be admitted. Even when your ED doctor determines you will be going home, it could take a couple of hours before you can leave the hospital. There are many reasons for this, some are: We have administered medication through an IV that is not completed. The medication given temporarily affects your ability to walk. We need to coordinate your safe transportation home, perhaps wait for a family member to pick you up. We need to arrange for special equipment/services for when you get home. Your specialist is in the hospital and wants to take a look at you or speak to you.
If you are going to be admitted, usually one of our hospitalists, that’s a physician who only sees patients admitted to the hospital, will write the order for the care unit that your condition requires, such as intensive care or medical surgical unit. You will be transferred to a room on that unit once a bed becomes available. Depending on how full the hospital is, this can extend your stay in the ED.
-Julie Tegay, RN
Q: Why can’t I have something to eat while I am waiting?
A: Patients are asked to refrain from eating until their test results are back in the event a surgical procedure is needed.
-Dr. Adam Wos
Q: Who will be treating me in the ED?
A: You will be seen by a physician, physician assistant, or nurse practitioner. The physician may be a resident, who is a licensed physician that works with our ED staff physicians.
-Julie Tegay, RN
Q: Will I see my own primary care physician?
A: Your ED physician may consult with your primary care physician. However, due to the increased demands of their practices, many primary care physicians have hospitalists speak with you. They will coordinate care with your primary care physician while you are here. After your discharge from Mather, your primary care physician will continue to direct your care.
-Phil Messina, RN
Q: Will I be admitted to the hospital?
A: You will be admitted based on your test results and diagnosis. Sometimes we need to observe patients for a while to determine if they need to be admitted or can be discharged home. This is called observation. Observation care seeks to treat patients whose condition doesn’t justify a hospital admission, but may still need follow-up, testing, or a little bit of “wait and see.” For example, a patient who shows up in the ED with stomach pain may just be constipated, or they may have appendicitis. Observation care helps to determine the level of care needed.
-Adam Wos, MD